 Midtown Manhattan
36 W 44th St Ste 1416 New York, NY 10036
Midtown Manhattan
36 W 44th St Ste 1416 New York, NY 10036
- (212) 621-7746
- text us
- BOOK ONLINE Call for Same Day Appointments
 Midtown Manhattan
36 W 44th St Ste 1416 New York, NY 10036
Midtown Manhattan
36 W 44th St Ste 1416 New York, NY 10036
When your veins become damaged in any way, whether they cause you pain or are just aesthetically unappealing, it may signal a serious health issue. A New York vein specialist like Dr. Febin Melepura at the Sports & Pain Institute of NY can tell you for sure if your health is at risk if you have vein pain. He then repairs the damage to get you back to looking and feeling better in no time. He relies on advanced techniques to relieve pain and restore your attractive skin. Call now for a consultation at his Midtown Manhattan office.
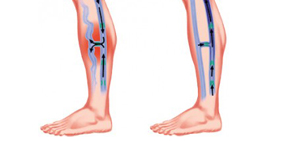 When visible or bulging veins concern you, whether you have associated pain or not, a thorough examination by a New York vein specialist provides you with a clear diagnosis that drives further treatment options. Dr. Febin Melepura at the Sports Injury & Pain Clinic NYC is a renowned interventional pain physician who couples state-of-the-art diagnostics with an eye for aesthetics to relieve your discomfort.
When visible or bulging veins concern you, whether you have associated pain or not, a thorough examination by a New York vein specialist provides you with a clear diagnosis that drives further treatment options. Dr. Febin Melepura at the Sports Injury & Pain Clinic NYC is a renowned interventional pain physician who couples state-of-the-art diagnostics with an eye for aesthetics to relieve your discomfort.
Vein treatment in NYC relies on a number of treatment options both to alleviate pain in legs and to improve the appearance of your skin. Tests such as a duplex ultrasound drive your doctor’s treatment recommendations. If you have no underlying or pressing health issues, such as venous insufficiency, you may at first be guided to try at-home treatment. These lifestyle remedies consist of:
Another common treatment for conditions like varicose veins involves wearing compression stockings. While you can purchase these socks at retail pharmacies over the counter to help improve blood flow in your legs, prescription high-strength stockings work best and are suited to your specific needs.
If the home care options don’t provide you with sufficient relief, your New York vein specialist moves on to other treatments — always starting with the least invasive. Procedures are done on an outpatient basis and may include:
Using the best vein treatment in NYC for your specific pain in your legs and for your unsightly veins, Dr. Melepura ensures that your treatment, no matter which one you need, causes minimal discomfort that lasts no more than a couple of days. The appearance of your skin typically improves within two weeks. Treatment for ulcers may take longer before you see a complete recovery, although your outcome is improved with compression therapy and follow-up visits.
Prepare for your initial appointment with a list of medications you’re taking, records of your medical history, estimates of your standing and sitting routines, and a summary of your dietary and exercise practices. Contact the Sports Injury & Pain Clinic NYC sooner rather than later for an appointment to resolve any medical and cosmetic issues with your veins. You’ll be on your feet and back in the game in no time!
Dr. Melepura took his time with me to discuss the issues with my veins. He was very thorough and presented me with multiple options. Very refreshing.
Nicholas AdamsLeg vein ablation is a procedure that uses either laser or radiofrequency waves to seal off damaged veins.
Vein ablation is used to treat venous reflux disease (backflow of blood). Vein ablation becomes necessary when your symptoms fail to improve with conservative treatments like compression stockings, exercise, weight loss, and lifestyle changes.
Vein ablation is a minimally-invasive office procedure. Minimally-invasive means one that doesn’t require a large cut. You may experience some discomfort, achiness, soreness, or tightness in the treated leg after the procedure, for which you can take Tylenol.
Yes, vein ablation is a safe procedure. Being less invasive, it doesn’t require significant cuts but tiny openings, and hence, doesn’t leave any large scars.
Vein ablation is a safe and well-tolerated procedure due to the recent advancements in the ablation technology. The rare complications include pain and bruising at the site of ablation, blood clot developing in the treated leg, changes in skin color over the ablated vein, and irritation of the nerves that lie close to the treated veins.
All insurance providers cover vein ablation when deemed medically necessary, i.e., when varicose veins cause bothersome symptoms like leg pain, heaviness, swelling, changes in skin color, and leg ulcers. However, vein ablation solely for cosmetic reasons is not considered medically necessary and is thus usually not covered by insurers.
The problematic vein is first mapped and marked under ultrasound guidance. The area is then numbed with a local anesthetic. A small nick is created in the skin of your leg. A wire is then inserted to help place a sheath (encasing device) into your vein. Your doctor will pass a catheter (a thin tube) into this sheath. The laser or radiofrequency energy is used to seal the faulty vein while slowly removing the catheter. The cut is finally covered with a bandaid, and a compression stocking is placed.
Vein ablation generally takes about 45–60 minutes. Additional sessions of vein ablation spaced over four to six weeks will be required if you have several faulty veins that need treatment.
Vein ablation is not painful. Most patients experience only mild discomfort that goes away in about a week or two after the procedure.
It takes about 12 months for the ablated veins to totally fade out. Bruising and skin color changes around the treated area may persist for weeks to months after vein ablation.
Vein ablation uses laser therapy or radio waves to heat and destroy the walls of the defective veins. Your body then absorbs the dead (scar) tissue on its own.
Yes, vein ablation helps improve your blood flow. The faulty leg veins cause the blood to flow in the wrong direction and pool in your legs. By sealing off these problematic veins, the blood flows through your circulation more efficiently using only your correctly functioning veins.
The risk of nerve damage is a lot less with vein ablation. The use of ultrasound guidance allows us to avoid the nerves that are close to the treated vein. However, heat exposure and large doses of the numbing medication can still induce nerve damage. The nerve will recover after a short time without any intervention.
People with advanced stages of venous reflux disease (backflow of blood) already have lymphedema. Lymphedema is a build-up of lymph (a clear-to-white fluid that runs throughout the lymphatic system of your body). In such patients, vein ablation can help improve lymphedema. However, another procedure for treating varicose veins called vein stripping and ligation carries a much higher risk of worsening lymphedema.
No, vein ablation actually helps improve high blood pressure. When your leg veins become faulty, the blood pools in them. This puts extra strain on your heart, which then needs to work harder to pump all of that pooled blood back up your body, thereby raising the blood pressure. Sealing the faulty leg veins by vein ablation helps redirect the blood flow to other healthier veins. This allows the blood to flow smoothly and prevent high blood pressure.
Your insurance provider will cover your treatment for varicose veins. Your ultrasound study needs to show that your veins are larger than they should be and that the blood is flowing in the opposite direction (reflux).
Varicose veins during pregnancy are treated by safe and conservative measures like wearing compression stockings, elevating the leg at times of rest, and watching your body weight. Vein ablation should be avoided during pregnancy but can be done as soon as six weeks into postpartum.
EVLA stands for endovenous laser ablation. Endovenous means that the entire procedure is carried out “inside” the faulty vein. Laser ablation is destroying the veins by laser therapy.

Febin Melepura, MD is a top rated, best in class interventional pain management doctor. He is a nationally recognized pain relief specialist and is among the top pain care doctors in New York City and the country. He is an award winning expert and contributor to a prominent media outlets.
Dr. Febin Melepura has been recognized for his thoughtful, thorough, modern approach to treating chronic pain and, among other accolades, has been named a “top pain management doctor in New York”, and one of “America’s Top Doctors™” for an advanced sports injury treatments.